Sarah Bagheni had a headache, fever, and itchy and unusual skin lesions for days, but she had no inkling that her symptoms might have been caused by mpox and that she might be another case in a growing global health emergency.
She also has no idea where to go to get medical help.
She and her husband live in the Bulengo displacement camp in eastern Congo, a region that is effectively ground zero for a series of mpox outbreaks in Africa.
This year's alarming rise in cases, including a new form of the virus identified by scientists in eastern Congo, led the World Health Organization to declare it a global health emergency on Wednesday. It said the new variant could spread beyond the five African countries where it had already been detected a timely warning that came a day before Sweden reported its first case of the new strain.
In the vast central African nation of Congo, which has had more than 96% of the world's roughly 17,000 recorded cases of mpox this year and some 500 deaths from the disease many of the most vulnerable seem unaware of its existence or the threat that it poses.
We know nothing about this, Bagheni's husband, Habumuremyiza Hire, said Thursday about mpox. I watch her condition helplessly because I don't know what to do. We continue to share the same room.
More From This Section
Millions are thought to be out of reach of medical help or advice in the conflict-torn east, where dozens of rebel groups have been fighting Congolese army forces for years over mineral-rich areas, causing a huge displacement crisis. Hundreds of thousands of people like Bagheni and her husband have been forced into overcrowded refugee camps around Goma, while more have taken refuge in the city.
Conditions in the camps are dire and medical facilities are almost nonexistent.
Mahoro Faustin, who runs the Bulengo camp, said that about three months ago, administrators first started noticing people in the camp exhibiting fever, body aches and chills symptoms that could signal malaria, measles or mpox.
There is no way of knowing how many mpox cases there might be in Bulengo because of a lack of testing, he said. There haven't been any recent health campaigns to educate the tens of thousands of people in the camp about mpox, and Faustin said he's worried about how many people might be undiagnosed.
Just look at the overcrowding here, he said, pointing to a sea of ramshackle tents. If nothing is done, we will all be infected here, or maybe we are already all infected.
Around 70% of the new mpox cases in the Goma area in the last two months that were registered at a treatment center run by Medair were from displacement camps, said Dr. Pierre Olivier Ngadjole, the international aid group's health advisor in Congo. The youngest of those cases was a month-old baby and the oldest a 90-year-old, he said.
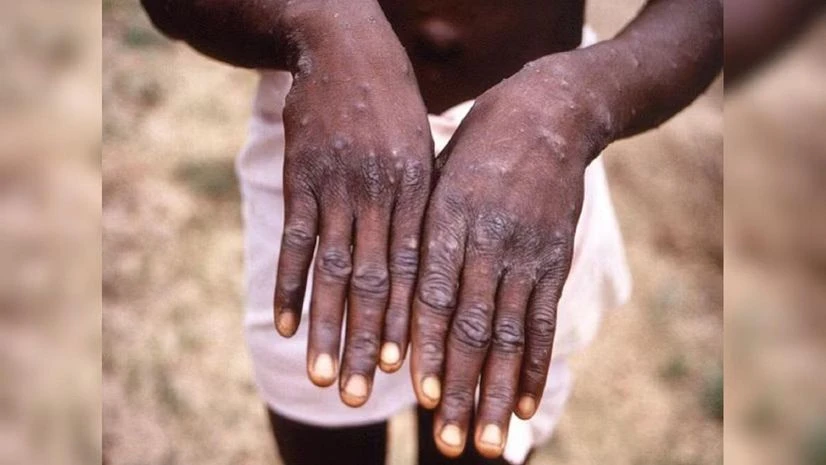
In severe cases of mpox, people can develop lesions on the face, hands, arms, chest and genitals. While the disease originated in animals, the virus has in recent years been spreading between people via close physical contact, including sex.
Bagheni's best hope of getting a diagnosis for her lesions is a government hospital that's a two-hour drive away. That's likely out of the question, given that she already struggles with mobility having previously had both her legs amputated.
Seven million people are internally displaced in Congo, with more than 5.5 million of them in the country's east, according the U.N. refugee agency. Congo has the largest displacement camp population in Africa, and one of the largest in the world.
The humanitarian crisis in eastern Congo has almost every possible complication when it comes to stopping an mpox outbreak, said Dr. Chris Beyrer, director of Duke University's Global Health Institute.
That includes war, illicit mining industries that attract sex workers, transient populations near border regions, and entrenched poverty. He also said the global community missed multiple warning signs.
We're paying attention to it now, but mpox has been spreading since 2017 in Congo and Nigeria, Beyrer said, adding that experts have long been calling for vaccines to be shared with Africa, but to little effect. He said the WHO's emergency declaration was late in coming, with more than a dozen countries already affected.
Beyrer said that unlike COVID-19 or HIV, there's a good vaccine and good treatments and diagnostics for mpox, but the access issues are worse than ever in places like eastern Congo.
In 2022, there were outbreaks in more than 70 countries around the world, including the United States, which led the WHO to also declare an emergency that lasted until mid-2023. It was largely shut down in wealthy countries within months through the use of vaccines and treatments, but few doses have been made available in Africa.
The new and possibly more infectious strain of mpox was first detected this year in a mining town in eastern Congo, about 450 kilometers (280 miles) south of Goma. It's unclear how much the new strain is to blame, but Congo is now enduring its worst outbreak yet and at least 13 African countries have recorded cases, four of them for the first time.
The outbreaks in those four countries Burundi, Kenya, Rwanda and Uganda have been linked to Congo's, and Doctors Without Borders said Friday that Congo's surge threatens a major spread of the disease to other countries.
Salim Abdool Karim, an infectious disease expert who chairs the Africa Centers for Disease Control and Prevention's emergency committee, said the Congo outbreak has a particularly concerning change, in that it's disproportionately affecting young people. Children under 15 account for 70% of cases and 85% of all deaths in the country, the Africa CDC reported.
Unlike the 2022 global outbreak, which predominantly affected gay and bisexual men, mpox now appears to be spreading in heterosexual populations.
All of Congo's 26 provinces have recorded mpox cases, according to the state-run news agency. But Health Minister Samuel-Roger Kamba said Thursday that the country doesn't have a single vaccine dose yet and he pleaded for "vigilance in all directions from all Congolese.
Dr. Rachel Maguru, who heads the multi-epidemic center at Goma's North Kivu provincial hospital, said they also don't have drugs or any established treatments for mpox and are relying on other experts such as dermatologists to help where they can. A larger outbreak around the city and its numerous displacement camps already overburdened with an influx of people would be terrible, she said.
She also noted a pivotal problem: poor and displaced people have other priorities, like earning enough money to eat and survive. Aid agencies and stretched local authorities are already wrestling with providing food, shelter and basic health care to the millions displaced, while also dealing with outbreaks of other diseases like cholera.
(Only the headline and picture of this report may have been reworked by the Business Standard staff; the rest of the content is auto-generated from a syndicated feed.)

)